It was 10pm on a busy shift in the emergency department. A 69 year-old man presented with sudden onset retrosternal chest pain radiating to his back. The pain lasted an hour and then resolved spontaneously. He drove himself to the ED for assessment. His initial ECG at triage was normal.
While in the ED, he developed severe back pain and diaphoresis. His ECG revealed evidence of an inferior myocardial infarction with ST elevation in AvR.
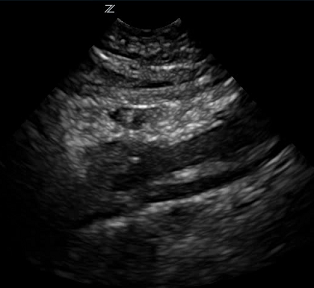
An aortic POCUS was performed which revealed the following:
This video demonstrates an intimal flap in the abdominal aorta consistent with an aortic dissection.
Based on this finding, a cardiac POCUS was performed:
This video demonstrates significant aortic regurgitation, concerning for evidence of a type A dissection. There was no evidence of a pericardial effusion. Based on this information, the cardiac surgery team was mobilized and the operating room was informed of the likely need for surgery.
The patient began complaining of some neck pain and headache. A scan of the right carotid artery was performed:
This scan reveals a dissection flap in the right common carotid artery. The patient was taken to CT scan and by the time the scan was done, the surgical team had arrived from home. The CT scan confirmed the presence of a type A aortic dissection extending into the carotids and down into the abdominal aorta. The patient was transported directly to the OR.
This case demonstrates how POCUS can help to expedite the care for patients with an aortic dissection. While transthoracic cardiac POCUS is not a sensitive test for dissection, it is highly specific and can be used to help rule in the diagnosis. With a type A dissection, a dissection flap can sometimes be seen on the parasternal long axis view above the aortic valve. Aortic regurgitation and presence of a pericardial effusion are also suggestive of a type A dissection. A dissection flap may also be visualized in the abdominal aorta if the dissection extends below the diaphragm.
If an aortic dissection is identified using POCUS, the surgical team can be notified of the patient and preparations for surgery can begin immediately. This can help expedite the transfer of patients to the operating room as soon as possible. Type A dissections have a mortality rate of 1-2% per hour, so any time saved in getting the patient to the operating room has the potential to reduce morbidity and mortality.
- An unusual headache - August 21, 2015
- Just another gastro – or is it? - May 11, 2015
- Knee vs Minivan - February 11, 2015


