


Point-of-Care Ultrasound
University of Toronto


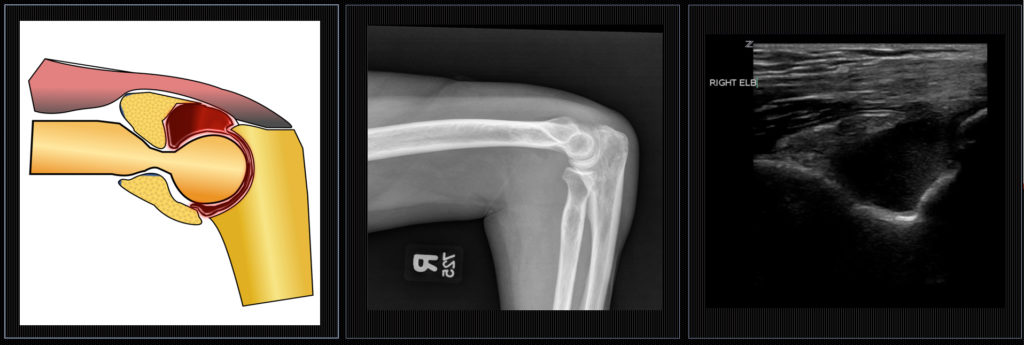
A 63 year-old lady fell outdoors after she was pulled over by her very bad dog. Apparently there was a squirrel.
She fell on her right side and her efforts to save her Starbucks landed her directly on her elbow.
Thanks to 4-point limb contact the dog stayed upright, the squirrel is still at large.
The FAST exam helped pave the way for Emergency point-of-care ultrasound. Compared to many emergency US applications still in their infancy, the FAST exam has been thoroughly studied, widely implemented, and has proven utility.
… sorry transcranial US…
The FAST has been around since the 1970’s and replaced DPL, it is very sensitive and even more specific. This makes it especially useful as a ‘rule-in’ test allowing expedition of surgery in unstable patients without the delays associated with advanced imaging.
Test Characteristics
Improved Outcomes
Finally it is teachable, portable and repeatable… not to mention FAST – taking an average of 2-4 minutes to perform
… but nothing is perfect…
Like every test the FAST can steer you wrong, false positives risk unnecessary CT scans, or even surgeries. False negatives can postpone further imaging and delay care. As the amount of US users increase, and no universally agreed upon training standards exist, it is important to ensure the continued accuracy of this critically important skill.
In Part I of this 2-part post I plan to discuss the cardinal features of ‘free fluid’ and how to avoid mistaking pee for blood (among other things).
Part II will follow with a review of the most common sources of false negatives I have encountered in teaching and practice, and how best to avoid them.
| Introductory Rotation |
| Advanced Elective |
| Ultrasound Fellowship |
| Faculty Guide |
| Schedule |
| IP Certification |
| Introductory Rotation Private Page |
| Advanced Elective Private Page |
| Ultrasound Fellowship |
| Ultrasound Fellowship Faculty |
| Ultrasound Fellows |
| Fellowship - Private Page |
| Basic Ultrasound |
| POCUS_Toronto Tutorials |
| Advanced Ultrasound |
| CEUS Quiz |
| Equipment Tutorials |
| Operating Manuals |